What Are The 5 Types Of Sleep Disorders?

Do you find yourself tossing and turning at night? You may be suffering from a rare sleep disorder. Many of us suffer from sleep disorders. It interferes with our ability to receive enough sleep.
Here, I aim to provide an overview of 5 sleep disorders. Knowing these, you can take action to enhance your sleep quality. It’s important to properly manage sleep disorders. They can impact physical and mental well-being and are not only a nocturnal issue.
We will discuss the treatments. I will give you certain tips to improve your sleep quality. Let’s explore.
Keep reading!
Sleep Disorders List
- Sleep apnea
- Insomnia
- Narcolepsy
- Restless Leg Syndrome (RLS)
- REM Sleep Behavior Disorder (RBD)
Now, let us explore each in detail!
5 Types of Sleep Disorder
Let me first throw some light on the 5 sleep disorders. Give it a read to enhance your knowledge on them.
1. Sleep Apnea
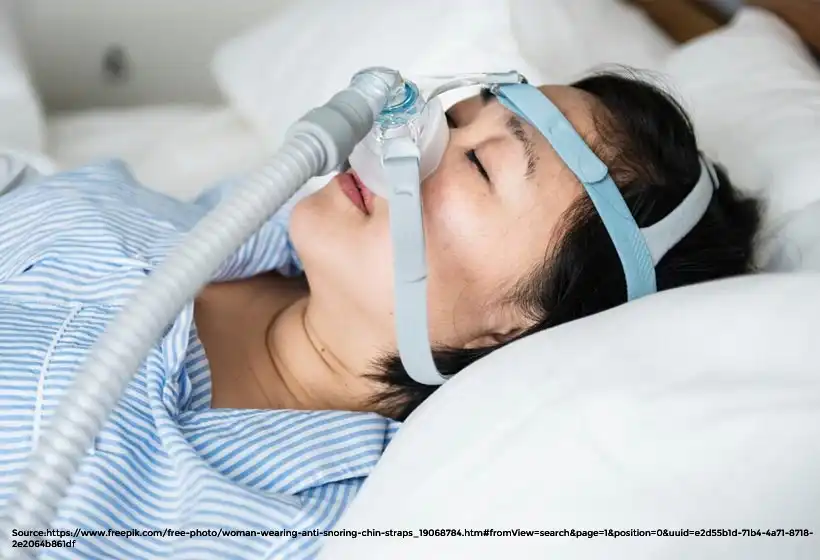
Sleep apnea is a common problem when you sleep. It makes you stop breathing for short periods while you’re asleep. This happens because your throat muscles relax. It blocks your airway, or because your brain doesn’t send the right signals.
Around 30 million Americans have obstructive sleep apnea, but many don’t know they have it. It can make you feel tired during the day, give you headaches in the morning, and leave your mouth dry.
There are two main types:
- Obstructive sleep apnea: This is when your throat muscles relax too much. It blocks your airway.
- Central sleep apnea: This is when your brain doesn’t send the right signals.
Sleep apnea can cause heavy snoring, and you might wake up suddenly because you’re choking or gasping for air.
There are treatments available, like using a Continuous Positive Airway Pressure (CPAP) machine. It helps keep your airway open while you sleep. Some people also use special mouthpieces or even have surgery to fix the problem.
Does Human Body Weight Affect Sleep Apnea?
When a person carries extra weight, especially around their neck and abdomen, it can increase the chances of having sleep apnea. Here’s why:
- Pharyngeal Fat: Extra weight can create fat deposits in the neck. It is known as pharyngeal fat. During sleep, the muscles in the throat rests. This can block the upper airway, making it harder to breathe properly.
This can result in snoring, a common symptom of a sleep disorder, because air is trying to squeeze through the narrowed airway, causing vibrations that make noise. - Abdominal Weight: Excess fat around the abdomen can put pressure on the chest wall, reducing the space available for the lungs to expand. This decreases the amount of air that can flow in and out of the lungs, making the upper airway to collapse during sleep, leading to episodes of sleep apnea.
- Body Mass Index (BMI): The risk of Obstructive Sleep Apnea (OSA) increases as the body mass index (BMI) rises. BMI measure body fat based on a person’s height and weight. Even a small increase in weight, like gaining just 10%, can significantly raise the risk of developing sleep apnea.
While excess weight is the primary factor contributing to sleep apnea in many cases, there are other less common causes as well. These include enlarged tonsils, anatomical features like a large neck or narrow throat, certain medical conditions like diabetes and thyroid disorders, acid reflux, lung diseases, and heart problems.
However, it’s important to note that a large proportion of adults with sleep apnea are overweight or obese.
So if you carry excess weight, especially around the neck and abdomen, your risk of developing sleep apnea can increase. This is by causing blockages in the upper airway and reducing lung capacity. This underscores the importance of having a healthy weight. It helps to minimize sleep apnea and its associated health problems.
Wait, does sleeping style have an effect in treating sleep apnea? Read more about it.
You can also learn about mattresses that help to relieve sleep apnea symptoms and ensure uninterrupted sleep.
2. Insomnia
Insomnia is when you have issue falling asleep or staying asleep. It is even when you really want to sleep and have plenty of time for it. It is an advanced stage sleep disorder. People with insomnia feel tired during the day. They may have trouble concentrating or doing things they need to do when they’re awake.
When these sleep problems happen at least three times a week for at least three months, it’s called chronic insomnia.
- Lots of adults go through periods where they have trouble sleeping, with up to two-thirds experiencing some form of insomnia now and then. Certain things can make insomnia more likely, like getting older, having less money, or feeling anxious or depressed.
Luckily, there are ways to help with insomnia.
- Therapy, sleep medications, and other methods can be used to lessen or even stop insomnia symptoms, so you can get the restful sleep you need to feel good during the day.
3. Narcolepsy
Narcolepsy is a sleep disorder. It makes people feel extremely tired during the day, even if they’ve slept enough at night. It can cause them to suddenly fall asleep without warning, which is called a “sleep attack.” These sleep attacks usually only last for a few minutes.
- In the United States, Narcolepsy affects about 1 in 2,000 people. Because of the sudden sleep attacks, people with Narcolepsy are at a higher risk of getting hurt in accidents.
- Narcolepsy happens because the brain has trouble controlling the sleep-wake cycle properly. Sometimes, people with Narcolepsy also experience something called cataplexy, where their muscles suddenly go weak, making them slump over or collapse.
But there are ways to manage Narcolepsy.
- Doctors can prescribe medications to help control the symptoms, and making changes to your daily routine and lifestyle can also make a big difference. With the right sleep disorder treatment, people with Narcolepsy can lead normal, active lives.
Do you have Narcolepsy? Read about important facts here.
4. Restless Leg Syndrome (RLS)
Restless Legs Syndrome, or RLS, is a sleep disorder. It causes uncomfortable sensations in the legs, like tingling or crawling feelings. These sensations create a strong urge to move the legs. It occurs especially when sitting or lying down, which can make it hard to fall asleep or stay asleep.
- Some common causes of RLS include pregnancy, Parkinson’s disease, and low levels of iron in the body, but often, the exact reason why someone develops RLS is unknown.
- RLS symptoms can also be made worse by things like drinking caffeine or taking certain medications, not just by resting.
Thankfully, there are ways to manage RLS.
- Making healthy changes to your sleep habits, diet, and exercise routine can help. Some people find relief from using special medical devices or taking medications prescribed by their doctor. By finding the right treatment, people with RLS can get better sleep and feel more comfortable during the day.
5. REM Sleep Behavior Disorder (RBD)
REM Sleep Behavior Disorder (RBD) is a sleep disorder where a person physically or vocally acts out their dreams. It happends during the rapid eye movement (REM) stage of sleep. They’re unaware of these actions while asleep.
- RBD can be isolated or secondary, meaning it’s either spontaneous or linked to other conditions like Parkinson’s disease or Narcolepsy.
- Symptoms include talking, shouting, kicking, or falling out of bed while asleep. RBD can lead to injury, so treatment is important.
What Causes Sleep Disorders?
What is sleep disorder? It can be caused by various factors that disturbs the natural cycle of sleep and wakefulness in the body. Here are some common causes:
- Medical Conditions: Underlying medical conditions such as heart disease, asthma, chronic pain, or nerve disorders can disrupt sleep patterns. It contribute to the development of sleep disorders.
- Mental Health Conditions: Mental health disorders like depression, anxiety, or stress can affect sleep quality and lead to sleep disorders. Similarly, conditions such as bipolar disorder or Post-Traumatic Stress Disorder (PTSD) can also disrupt sleep.
- Genetic Factors: Some sleep disorders may have a genetic component. This means they can run in families. Genetic mutations or variations may predispose individuals to certain sleep disorders.
- Medication Side Effects: Certain medications can interfere with normal sleep patterns. It contribute to the development of sleep disorders. This includes medications for conditions like hypertension, asthma, depression, or allergies.
- Shift Work: Working irregular or overnight shifts can disrupt the body’s natural sleep-wake cycle, leading to sleep disorders. It is called as shift work sleep disorder.
- Substance Use: Consumption of substances like caffeine or alcohol close to bedtime can interfere. It hampers the ability to fall asleep or maintain sleep throughout the night, contributing to sleep disorders.
- Imbalance of Brain Chemicals: Low levels of certain neurotransmitters or minerals in the brain, such as serotonin or magnesium, can affect sleep regulation and contribute to sleep disorders.
- Unknown Causes: In some cases, the exact cause of a sleep disorder may not be known. Research is ongoing. It will help to understand the underlying mechanisms and factors contributing to various sleep disorders.
Overall, the answer to what causes sleep disorders can be complex and multifaceted. It involvs a combination of biological, psychological, environmental, and lifestyle factors. Identifying as well as addressing the underlying causes is crucial for effectively managing and treating sleep disorders.
Other Causes include:
- Injury In Humans And Sleep Disorder
Traumatic Brain Injury (TBI) is causes sleep disorders, with many patients experiencing long-term sleep dysfunction following the injury. Research suggests that alterations in the hormone melatonin, which regulates sleep and circadian rhythms, may be linked to these sleep disturbances in individuals with TBI.
- Role of Melatonin in Sleep
Melatonin plays a important role in regulating the sleep-wake cycle and has been recognized as a neuro-protective anti-inflammatory agent. However, the exact mechanisms underlying its involvement in sleep disorders after TBI are still being explored.
There is an interesting role in melatonin’s biochemical properties and its potential therapeutic benefits in managing sleep disorders associated with TBI. Melatonin has been investigated for its role in promoting sleep, protecting the brain from further damage, and modulating circadian rhythms disrupted by TBI.
Despite increasing interest in using melatonin to treat insomnia following TBI, there is a lack of standardization and rigor in research, resulting in non-generalized data and unclear treatment recommendations.
Moving forward, there is a need for more rigorous and standardized research to fully understand the therapeutic potential of melatonin in managing sleep disorders in individuals with TBI. This includes exploring its neuroprotective properties, its ability to promote sleep and its role in regulating circadian rhythms.
By better understanding the biochemical properties of melatonin and its effects on sleep and brain function, clinicians may develop more effective strategies for managing sleep disorders in individuals with TBI.
Are you curious about Melatonin and Its Effect On Sleep/Wake Cycles? Read on.
Risk Factors of Rare Sleep Disorders

Several factors can enhance the risk of developing sleep disorders. These risk factors include:
- Underlying Health Conditions: There are certain medical conditions such as heart disease, asthma, chronic pain, or mental health disorders. It is like depression or anxiety which can increase the risk of experiencing sleep disorders.
- Stress: High levels of stress can disrupt sleep patterns. It contributes to the development of rare sleep disorders.
- Family History: Having a family history of sleep disorders can predispose individuals to experiencing similar sleep problems themselves. Genetic factors may play a role in certain sleep disorders.
- Gender: Research suggests that women are more likely to experience sleep disorders compared to men and people assigned male at birth. Hormonal changes during menstruation, pregnancy, and menopause can affect sleep patterns in women.
- Age: Sleep disorders are more common among older adults, with about half of all adults over the age of 65 experiencing some type of sleep disorder. Changes in sleep architecture and medical conditions with age can contribute to sleep disturbances in older adults.
Considering these risk factors can help individuals and healthcare professionals. It will identify those who may be at higher risk of developing sleep disorders and take proactive steps to address sleep-related issues.
By addressing underlying health conditions, managing stress, and adopting healthy sleep habits, individuals can reduce their risk of experiencing sleep disorders and improve overall sleep quality and well-being.
What Causes Sleep Disorders in Adults?
1. Shift Work Disorder

Shift work disorder affects some individuals who work late at night or early in the morning, disrupting their natural sleep-wake cycle. It causes advanced phase sleep disorder.
Because they must sleep during the day and work at night, their body’s internal clock, known as circadian rhythms, becomes misaligned with their work schedule.
- This misalignment can cause people with shift work disorder to feel excessively tired while at work and struggle to get enough sleep during their daytime rest period. Essentially, their bodies don’t know when to feel alert or sleepy because of the irregularity in their schedule.
- Statistics show that at least one-third of shift workers have shift work disorder. On average, individuals with shift work disorder get 90 minutes less sleep compared to those who work day shifts.
- Treatment for shift work disorder focuses on implementing strategies to promote alertness while at work and encourage quality sleep during the limited daytime hours available for rest. This may include techniques such as optimizing sleep environments, practicing good sleep hygiene, and potentially using medications or supplements to aid sleep.
By addressing these factors, individuals with shift work disorder can better manage their symptoms.
2. Non-24-Hour Sleep Wake Disorder
Non-24-hour sleep-wake Disorder is a condition where an individual’s internal body clock, known as circadian rhythms, doesn’t reset every 24 hours as it does for most adults. Instead, their circadian rhythms are either shorter or longer than 24 hours. It causes rare sleep disorder symptoms.
This means affected individuals progressively shift their sleep and wake times earlier or later each day, typically by one to two hours.
- This disorder affects people who are blind and unable to perceive light, which is a crucial cue for resetting circadian rhythms in most people. Without this cue, their internal body clocks drift out of sync. This is with the 24-hour day-night cycle.
- People with non-24-hour sleep-wake disorder often experience cycles where they sleep during the day for days or weeks, followed by periods of sleeping at night. This irregular sleep pattern can lead to significant disruptions in daily life and functioning.
Non-24-hour sleep-wake disorder is classified as one of the six circadian sleep-wake rhythm disorders, which involve disruptions in sleep timings relative to the 24-hour day-night cycle.
- Management of this disorder typically involves strategies to help regulate sleep patterns, such as exposure to bright light at specific times of day and the use of medications to promote sleep and wakefulness at appropriate times.
Rare Sleep Disorders
Now that we have learnt about the most common sleep disorders and the ones most prevalent in adults, let’s read about some rare types.
1. Bipolar Disorder
Bipolar disorder is a mental health condition. It is characterized by extreme mood swings. It include emotional highs (mania or hypomania) and lows (depression). Sleep disturbance is a symptom of bipolar disorder, and it plays a significant role in both manic and depressive episodes.
- Individuals with bipolar disorder may experience a reduced need for sleep. They may feel energized, restless, and hyperactive, making it difficult for them to fall asleep or stay asleep.
Despite the lack of sleep, they may not feel tired and may engage in activities for extended periods without feeling the need to rest. - Conversely, during depressive episodes, insomnia or hypersomnia can occur nearly every day. Insomnia is difficulty in falling asleep or staying asleep. Hypersomnia involves excessive daytime sleepiness and long periods of sleep, yet still feeling tired during the day.
- The interrelation between bipolar disorder and sleeplessness is complex and multifaceted. Sleep disturbances can exacerbate mood swings and increase the severity of bipolar symptoms.
Conversely, manic or depressive episodes can disrupt sleep patterns, leading to further sleep disturbances and worsening of bipolar symptoms.
Medications & Treatment
Fluoxetine medication is commonly used to treat depression, including depressive episodes associated with bipolar disorder. It is called selective serotonin reuptake inhibitor (SSRI) antidepressant. It works by enhancing the levels of serotonin in the brain. This can elevate mood and alleviate symptoms of depression.
However, fluoxetine and other antidepressants may also affect sleep patterns, potentially causing insomnia or other sleep disturbances as side effects.
It’s essential for individuals with bipolar disorder. It work closely with their healthcare providers. It helps to manage their symptoms effectively. You may go to a sleep disorder therapist.
Treatment may consists of a combination of medication, therapy, lifestyle modifications, and strategies to promote healthy sleep habits. By addressing sleep disturbances and managing bipolar symptoms, individuals can improve their overall quality of life and well-being.
2. Somatic Symptom Disorder
Somatic Symptom Disorder (SSD) is a condition where individuals experience distressing physical symptoms that cannot be fully explained by medical conditions. These symptoms often include localized or generalized pain, fatigue, and sleep disturbances.
The relationship between somatic symptom disorder and sleep disorders is complex and bidirectional.
- Patients diagnosed with somatic symptom disorders frequently report sleep disturbances which include insomnia and Obstructive Sleep Apnea (OSA). Research suggests that chronic pain, such as that experienced in somatic symptom disorders, can be associated with sleep disturbances.
- For instance, localized pain in areas like the oro-facial region or limbs has been reported in patients with OSA and Restless Leg Syndrome, respectively. Similarly, generalized pain is often reported by individuals with insomnia and circadian rhythm disorders.
- While there is a coexistence of somatic symptoms, pain, and sleep disorders, establishing the direction of causality is challenging due to limited research. However, specific patterns in sleep disturbances have been identified among patients with chronic pain syndromes like Fibromyalgia and Chronic Fatigue Syndrome. Polysomnography, a sleep study, has revealed distinct signatures in sleep parameters and micro-architecture among these patients.
Addressing sleep disturbances in these patients may not only improve sleep quality but also alleviate pain and overall distress associated with somatic symptom disorder.
Thus, the relationship between somatic symptom disorder and sleep disorders involves a complex interplay of symptoms and underlying mechanisms. Recognizing and addressing sleep disturbances as part of the management of somatic symptom disorder can lead to better outcomes and a good quality of life for affected individuals.
3. Cataplexy
Cataplexy is a loss of voluntary muscle tone triggered by intense emotions such as laughter, excitement, anger, or fear. It is strongly associated with Narcolepsy, an advanced phase sleep disorder characterized by excessive daytime sleepiness and sleep paralysis.
- Approximately two-thirds of individuals with Narcolepsy also experience cataplexy, making it a defining feature of the condition.
- Laughter is the most common trigger of cataplexy, although other strong emotions can also induce episodes. Cataplexy typically occurs during waking hours, distinguishing it from other symptoms of Narcolepsy, which occur during sleep.
- During a mild episode of cataplexy, there may be subtle signs of muscle weakness, such as drooping eyelids. In more severe cases, a person may experience a complete loss of muscle control, leading to a total body collapse.
- It’s important to note that while cataplexy shares some similarities with seizure disorders, it is a distinct condition and can sometimes be misdiagnosed as such.
- While there is no cure for cataplexy, it can be managed with medications along with lifestyle modifications aimed at reducing potential triggers. Medications such as antidepressants and sodium oxybate are commonly used to help control cataplexy episodes and enhance the quality of life for individuals with Narcolepsy.
Cataplexy is a unique and potentially debilitating symptom of Narcolepsy, characterized by sudden muscle weakness triggered by strong emotions. With proper management and treatment, individuals with cataplexy can better control their symptoms and lead fulfilling lives.
Sleep Deprivation & Related Health Problems
Not getting enough sleep can have consequences beyond just feeling tired during the daytime. Here are some of the effects of sleep deprivation on health and well-being:
- Cognitive Impairment: Sleep deprivation can impair cognitive function, making it difficult to learn, remember information, or make decisions. This can impact academic or work performance and overall productivity.
- Mood Changes: Lack of sleep can lead to irritability, mood swings, and changes in personality. It can also enhance symptoms of anxiety and depression, making it harder to cope with stressors in daily life.
- Impaired Motor Skills: Sleep deprivation can decrease reaction times and coordination, increasing the risk of accidents and injuries. This occurs especially while driving or operating machinery.
- Health Conditions: Chronic sleep deprivation causes increased risk of various health conditions which includes obesity, type 2 diabetes, heart disease, and hypertension. Sleep plays a crucial role in regulating hormones. It control appetite and metabolism, and disruptions in sleep patterns can cause weight gain and metabolic dysfunction.
- Mental Health Disorders: Lack of sleep is linked to an increased risk of developing depression and anxiety disorders. Sleep disturbances can disrupt the balance of neurotransmitters in the brain, contributing to mood disorders.
- Cognitive Decline: Chronic sleep deprivation has been associated with an increased risk of dementia and cognitive decline in older adults. Adequate sleep is essential for memory consolidation and brain health.
While rare, severe sleep disorders can pose life-threatening risks. Conditions such as sleep apnea cause pauses in breathing during sleep. It can lead to serious complications if left untreated, including cardiovascular problems and even death.
You need to prioritize quality sleep, which is essential for maintaining physical and mental well-being. Establishing healthy sleep habits and seeking treatment for sleep disorders can help prevent the negative consequences of sleep deprivation and promote overall health and vitality.
Sleep Disorders Symptoms
Symptoms of sleep disorders can vary depending on the type of disorder, but commonly reported signs include:
- Wakefulness or Difficulty Falling Asleep: It may take more than 30 minutes to fall asleep regularly, or you may struggle to initiate sleep despite feeling tired.
- Trouble Staying Asleep: You may experience frequent awakenings during the night, finding it challenging to maintain uninterrupted sleep throughout the night. Waking up often in the middle of the night and having difficulty falling back asleep is also common.
- Snoring, Gasping, or Choking: These symptoms may occur during sleep, particularly in conditions such as obstructive sleep apnea, where breathing may be temporarily interrupted during sleep.
- Restless Legs Syndrome (RLS): You may feel a strong urge to move your legs when you relax, and this sensation is relieved by movement.
- Sleep Paralysis: Some individuals may experience a temporary inability to move or speak when waking up or falling asleep.
During the daytime, additional symptoms may manifest due to inadequate sleep, including:
- Excessive Daytime Sleepiness: Feeling excessively tired during the day, leading to frequent daytime naps or unintentionally falling asleep during routine activities.
- Difficulty Concentrating or Paying Attention: Sleep disturbances can impair cognitive function, making it challenging to focus, retain information, or perform tasks effectively.
- Mood Changes: Sleep deprivation can contribute to irritability, mood swings, and difficulty managing emotions.
- Impaired Performance: Difficulties meeting deadlines or performance expectations at work, school, or daily tasks may occur due to sleep-related impairments in cognitive function and alertness.
- Increased Risk of Accidents: Sleepiness and impaired cognitive function can increase the risk of accidents, falls, or errors in judgment.
If you experience persistent symptoms of sleep disturbances that interfere with your daily activities and quality of life, it’s essential to seek evaluation and guidance from a healthcare provider. They can help diagnose any underlying sleep disorders and recommend appropriate treatment strategies to improve your sleep quality and overall well-being.
Diagnosis of Sleep Disorders
Diagnosing sleep disorders typically involves a comprehensive evaluation by a healthcare provider and may include various tests and assessments.
Here’s an overview of how sleep disorders are diagnosed:
1. Physical Examination and Review of Symptoms
Your healthcare provider will conduct a physical exam and review your medical history, including any symptoms related to sleep disturbances. They will inquire about your sleep patterns, daytime symptoms, and any underlying health conditions that may contribute to sleep problems.
2. Sleep Diary
Keeping a sleep diary can provide valuable insights into your sleep habits and patterns. You’ll record information such as bedtime, time to fall asleep, awakenings during the night, duration of sleep, and daytime naps. Additionally, you’ll note any factors that may affect sleep, such as caffeine or alcohol consumption, stress levels, or medication use.
3. Actigraphy
Some individuals may be asked to wear a device called an actigraph, typically worn on the wrist, which records movement and activity patterns. This device helps track sleep-wake cycles over an extended period, providing objective data on sleep duration and quality.
4. Sleep Study (Polysomnogram)
If necessary, your primary care provider may refer you to a sleep specialist for a sleep study, also known as a polysomnogram. During a sleep study, you’ll spend a night in a sleep laboratory or specialized sleep center, where various body functions are monitored while you sleep.
This includes measurements such as brain activity, eye movements, muscle activity, heart rate, and breathing patterns. The data collected during the sleep study helps healthcare providers evaluate sleep architecture and identify any abnormalities or sleep disorders.
5. Blood Tests or Imaging Tests
In some cases, blood tests or imaging tests may be ordered to assess for underlying medical conditions that could contribute to sleep disturbances, such as thyroid disorders or sleep-related breathing disorders.
After gathering all relevant information and test results, your healthcare provider will analyze the data to make a diagnosis and develop a personalized treatment plan tailored to your specific sleep disorder and individual needs. Working closely with your healthcare team, you can address sleep-related issues effectively and improve your overall sleep quality and well-being.
Sleep Disorders Treatment
Treatment for sleep disorders varies depending on the specific type of disorder and individual needs.
Here’s an overview of common treatment options:
- Lifestyle and Behavioral Changes: Your healthcare provider may recommend changes to your sleep routine and habits to promote better sleep hygiene. This includes maintaining a regular sleep schedule, creating a comfortable sleep environment, and practicing relaxation techniques before bedtime.
- Cognitive Behavioral Therapy (CBT): CBT for insomnia is a structured therapy that aims to address the underlying factors contributing to sleep difficulties. It involves techniques such as cognitive restructuring, stimulus control, and sleep restriction to improve sleep quality and duration.
- Medications: Depending on the type of sleep disorder, medications may be prescribed to alleviate symptoms and improve sleep. Common medications include:
- Insomnia: Sleep aids such as melatonin, zolpidem, zaleplon, eszopiclone, ramelteon, suvorexant, lamborexant, or doxepin.
- Restless Legs Syndrome: Medications like gabapentin, gabapentin enacarbil, or pregabalin.
- Narcolepsy: Stimulants or wake-promoting medications such as modafinil, armodafinil, pitolisant, mixed salt or sodium oxybate, and solriamfetol.
- Continuous Positive Airway Pressure (CPAP) Therapy: CPAP therapy is a common treatment for obstructive sleep apnea. It involves wearing a mask connected to a machine that delivers a continuous flow of air to keep the airway open during sleep.
- Light Therapy: Light therapy may be recommended for sleep disorders related to circadian rhythm disturbances, such as delayed sleep phase syndrome or seasonal affective disorder. Exposure to bright light, particularly in the morning, can help regulate the sleep-wake cycle.
- Surgical Interventions: In some cases of sleep apnea, surgical procedures may be considered to address anatomical abnormalities that contribute to airway obstruction during sleep.
It’s essential to work closely with your healthcare provider to determine the most appropriate treatment for your sleep disorder. They will consider factors such as the type and severity of your symptoms, medical history, and individual preferences when developing a personalized treatment plan.
Additionally, your doctor will monitor your progress and make adjustments to your treatment as needed to optimize sleep quality and overall well-being.
Sleeping Problems Solutions: Top Tips

Improving sleep quality involves adopting healthy sleep hygiene habits and creating an optimal sleeping environment. Here are some tips to enhance your sleep quality:
- Tip 1: Create a Comfortable Sleep Environment: Ensure your bedroom is conducive to sleep by keeping it cool, quiet, and dark. Consider using earplugs or white noise machines to mask disruptive sounds, and use blackout curtains or a sleep mask to block out light.
- Tip 2: Minimize Stress: Practice stress-reduction techniques before bedtime, such as journaling, meditation, or deep breathing exercises. Avoid engaging in stressful activities or worrying thoughts close to bedtime.
- Tip 3: Reserve Your Bed for Sleep and Intimacy: Avoid using your bed for activities other than sleep and intimacy. Refrain from watching TV, working, or eating in bed, as these activities can disrupt your sleep environment.
- Tip 4: Establish a Regular Bedtime Routine: Develop a relaxing bedtime routine to signal to your body that it’s time to wind down. This may include activities like taking a warm bath, listening to calming music, or reading a book. Consistency is key, so aim to go to bed and wake up at the same time each day, even on weekends.
- Tip 5: Limit Screen Time Before Bed: Avoid using electronic devices such as smartphones, tablets, or computers in the hour leading up to bedtime, as the blue light emitted can interfere with your body’s natural sleep-wake cycle.
- Tip 6: Avoid Watching the Clock: Obsessively checking the time can increase anxiety about sleep, making it harder to fall asleep. Turn your clock away from view or place your phone screen-side down to minimize clock watching.
- Tip 7: Engage in Regular Exercise: Regular physical activity can promote better sleep, but avoid vigorous exercise close to bedtime as it may stimulate your body and make it harder to fall asleep.
- Tip 8: Invest in Quality Bedding and Mattress: Your bedding and mattress play a significant role in determining your comfort and support while you sleep. Choose a mattress and pillows that are comfortable and supportive, providing proper alignment for your spine and reducing pressure points.
Opt for high-quality bedding materials that promote breathability and temperature regulation.
I suggest you incorporate these tips. It will help improve sleep quality and promote overall well-being. If sleep problems persist, consult with a healthcare provider.
FAQs on Sleep Disorders
Q1. What are the five major sleep disorders?
- Five primary sleep disorders include Restless Legs Syndrome (RLS), characterized by leg movement due to discomfort; Insomnia, difficulty falling or staying asleep; REM Sleep Behavior Disorder (RBD); Sleep Apnea, interrupted breathing during sleep; and Narcolepsy, sudden daytime sleepiness.
Q2. Is a sleep disorder a mental illness?
- Sleep disorders like insomnia often signal underlying health issues rather than standalone mental illnesses. They can stem from lifestyle factors or other medical conditions, necessitating investigation and treatment by medical professionals.
Q3. Do sleep disorders go away?
- Sleep disorders typically dissipate with treatment addressing their root causes. Effective management often combines medical interventions with lifestyle adjustments. Identifying and addressing underlying issues is key to resolving sleep disturbances.
Q4. How do I fix my sleep disorder?
- Improving sleep habits involves optimizing your sleep environment, maintaining a proper sleep schedule, avoiding stimulants, and engaging in regular daytime physical activity, among other strategies.
Q5. What is sleep anxiety?
- Sleep anxiety entails apprehension or stress surrounding sleep onset or maintenance, often intertwined with broader mental health issues. Addressing anxiety and sleep problems is important, as they can exacerbate each other but are treatable conditions.
Q6. Is bipolar disorder a sleep disorder?
- Bipolar disorder often involves significant sleep disturbances, including reduced need for sleep during manic episodes and insomnia or hypersomnia during depressive phases.
Q7. What does lack of sleep do to the brain?
- Sleep deprivation diminishes protective factors for neurons, impairing cognitive function. Prolonged sleep loss raises the risk of neurological diseases like Alzheimer’s, emphasizing the critical importance of adequate sleep for brain health.
Q8. Why am I so tired but can’t sleep?
- Insomnia, characterized by difficulty sleeping despite exhaustion, can result from various factors such as chronic pain, medication side effects, or lifestyle choices like irregular sleep schedules.
Q9. Why do I struggle to wake up?
- Struggles with waking up can stem from parasomnias like sleepwalking, sleep apnea with interrupted breathing, or overall sleep deficiency, including poor sleep quality or insufficient sleep duration.
Q10. Why is my mind racing at night?
- Night-time racing thoughts may arise from stressors, anxiety disorders, or stimulants like caffeine. Managing nighttime anxiety involves addressing underlying stressors and adopting relaxation techniques to promote restful sleep.
Disclaimer
The information here provides general guidance. It is not a substitute for professional advice. It supplements knowledge but doesn’t diagnose sleep or health issues. Before adjusting your sleep habits, seek personalized care from a healthcare provider.

